A recent study found that daratumumab (DARA) monotherapy was well tolerated and effective at preventing or delaying progression of high-risk smoldering multiple myeloma (SMM) to active MM when compared with active monitoring. Patients receiving DARA experienced longer time to first-line treatment for MM. Preliminary data from the AQUILA study were presented at the ASH Annual Meeting.
“SMM is an asymptomatic precursor disorder to active MM without approved treatment options,” wrote the authors, led by Meletios-Athanasios Dimopoulos of the National and Kapodistrian University of Athens and Alexandra General Hospital in Greece. “These results strongly support the benefit of early intervention with DARA monotherapy versus active monitoring, the current standard of care, in patients with high-risk SMM.”
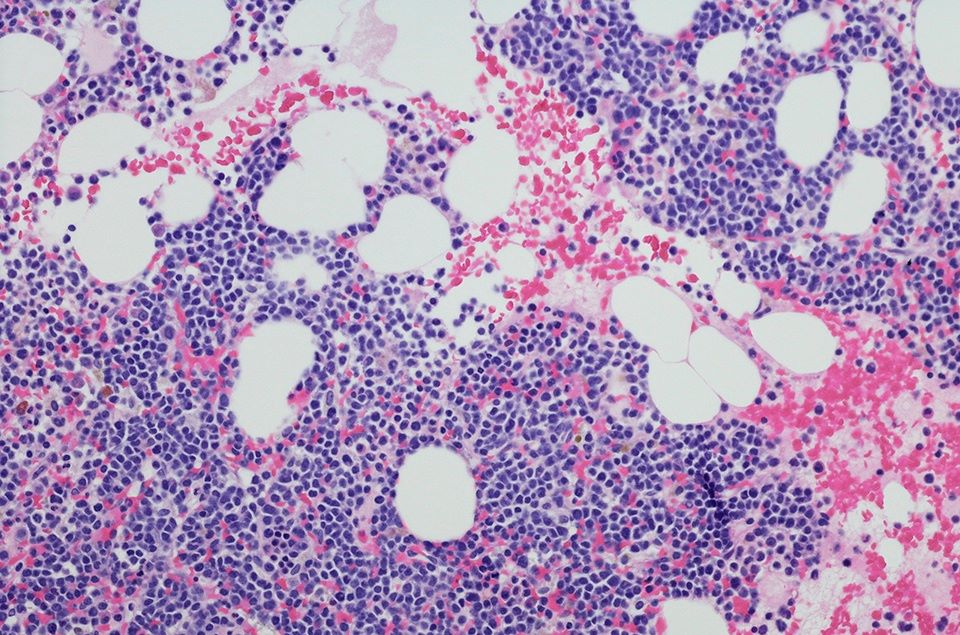
DARA is a monoclonal antibody that binds to CD38, a protein found in cancer cells and some immune cells. The immunotherapeutic is approved as monotherapy for relapsed/refractory MM and in combination with standard-of-care regimens for relapsed/refractory MM and newly diagnosed MM. The phase 2 CENTAURUS study noted promising results of DARA monotherapy in patients with intermediate- or high-risk SMM. Subsequently, the phase 3 AQUILA study assessed whether DARA could delay progression to MM.
The study enrolled390 patients with a confirmed diagnosis of high-risk SMM for five years or less. Patients were randomized to receive DARA (n=194) or active monitoring (n=196), and the groups were balanced by age (median, 64 years; range, 31–86 years) and time since diagnosis (median, 0.72 years; range, 0–5.0 years). Those in the DARA group received the drug in 28-day cycles until cycle 39 (equal to 36 months) or disease progression, whichever came first. Treatment occurred weekly in cycles 1 and 2, every two weeks in cycles 3 through 6, and every four weeks thereafter. Median DARA treatment duration was 38 cycles (35 months).
At a median follow-up of 65.2 months (range, 0–76.6), those receiving DARA had significantly better progression-free survival (PFS). That group did not reach median PFS versus 41.5 months among those receiving active monitoring. The researchers estimated 60-month PFS rates to be 63.1% versus 40.8%, respectively. The overall response rate was 63.4% with DARA versus 2% with active monitoring. Furthermore, DARA appeared to delay the need for first-line treatment for MM; at the time of data analysis, 64 (33%) patients in the DARA group and 102 (52%) in the active monitoring group had started first-line MM treatment.
40.4% of DARA recipients experienced grade 3/4 treatment-emergent adverse events (TEAEs), the most common of which was hypertension. Only 5.7% discounted DARA due to TEAEs, and only 1% died due to TEAEs.The study population had a total of 41 deaths (15 in the DARA group and 26 in the active monitoring group).
https://ash.confex.com/ash/2024/webprogram/Paper201057.html
Reference
Dimopoulos M-A, Voorhees PM, Schjesvold F, et al. Phase 3 randomized study of daratumumab monotherapy versus active monitoring in patients with high-risk smoldering multiple myeloma: primary results of the Aquila Study. Abstract #773. Presented at the 66th American Society of Hematology Annual Meeting and Exposition; December 7–10, 2024; San Diego, California.